Common challenges faced by sedationists in the IR department
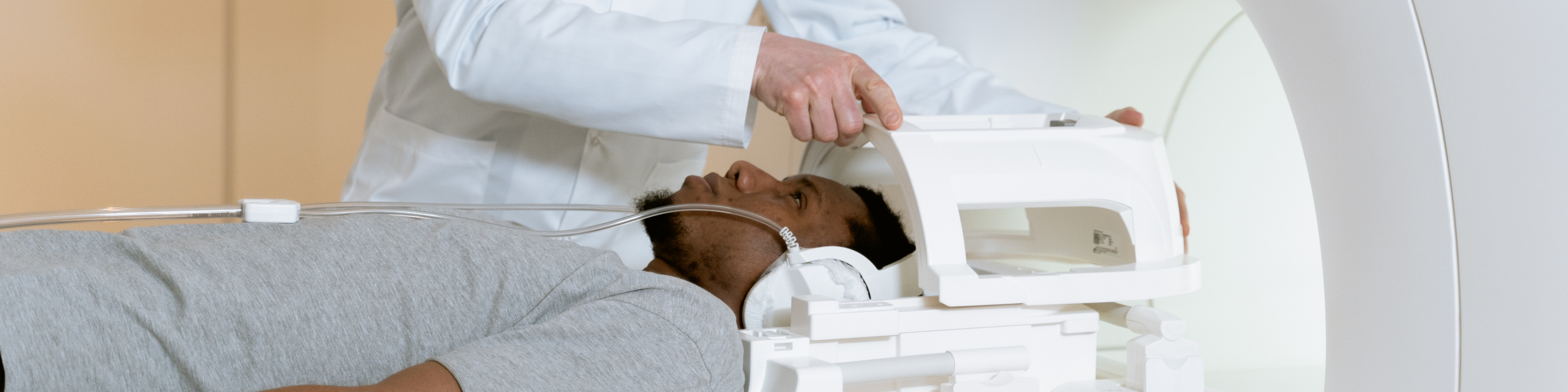
Over the last few years, we’ve witnessed an increase in the number of radiology procedures performed under sedation. But we have also seen an increase in the amount of comorbidities patients are presenting with for these procedures. Non-anaeshetist sedationists are faced with a need to develop sedation related skills to keep these patients safe, but also to implement safe sedation policies in their departments. In this blog, we discuss common challenges faced by sedationists in the IT department.
Challenges related to procedures
As mentioned above, we have seen more complex and/or long radiological techniques being performed. Advanced in technology have allowed these minimally invasive procedures to be more attractive to patients and clinicians alike. However, with long or complex procedures, sedation also becomes more complex and practitioners need to choose appropriate sedative drugs and administration methods suitable for those procedures.
It is also recognised that procedures like image-guided biopsies can be uncomfortable and anxiety-inducing. Patients may be asked to hold their breath when instructed. Clinicians must maintain light sedation levels to help alleviate discomfort while avoiding oversedation which can be challenging [4].
For these reasons, capnography is even more important in helping detect respiratory compromise and keep patients safe.
Challenges related to patients
Patients requiring IR procedures are presenting with more complex problems. A study has found that patients undergoing IR procedures are more likely to be obese than the general population [3]. This presents a particular problem in sedation because high BMI is a risk factor for sedation-related complications, including hypoxia [4]. To minimize these risks, clinicians need to personalize sedation with important adjustments for obese patients [3].
Another challenge related to patients relates to those patients with such comorbidities that they are not qualified for surgery in the OR and may instead undergo IR procedures and receive sedation [6]. These may include patients with serious conditions such as COPD or advanced cancer [8,7]. With increased comorbidities, the risk of sedation-related complications also increase.
Challenges related to staff
There are also several challenges related to staff working in IR. Historically, staff weren’t involved in patient’s pre assessment, which limits their ability to prepare for eventual complications and from time to time find that certain patients are not suitable for sedation by non-anaesthetists. Equally, many staff are also not familiar with the use of capnography, still relying solely on pulse oximetry to detect respiratory compromise. More training on capnography is required for staff working in IR.
Another challenge is related to the lack of formal training which is one of the main reasons for morbidity and mortality in sedation practice. Since the Academy of Medical Royal Colleges issued sedation guidelines in 2013, formal training has been a requirement, but there has been a slow uptake of these guidelines and still many staff are caring for sedated without formal training.
And finally, the lack of resources is also a common problem. A minimum of 3 members of staff is required when practicing moderate sedation, but in many hospitals, staff are still struggling to have a dedicated sedation practitioner for each procedure.
